-

Opioids and Young Adults in Alaska: Access, Consumption, Consequences, and Perceptions
Andrew Richie, Bridget Hanson, and Kathryn E. Davis
Over the past 5 years, numerous state and local activities have targeted opioid prevention among Alaskans, particularly youth and young adults. While surveillance data exists for youth, no specific data exists for opioid behaviors and perceptions among Alaskan young adults. Researchers at the University of Alaska Anchorage Center for Behavioral Health Research and Services conducted surveys in 2016 and 2019 to gather information on awareness, opioid and heroin use, social and retail access, and risk perceptions. At each timepoint, Alaskans age 18-27 were randomly selected and invited to participate. Response rates for the surveys were 10.4% and 12.8%, respectively. Survey data were weighted for gender and borough in order to represent Alaska’s population of young adults. Changes from 2016 to 2019: Increase in seeing awareness messages about opioids Increase in rating prescription opioid misuse and heroin use as problems in community. Increase in perceived risk from misusing opioids or using heroin. Among those who had been prescribed opioids in the past three years: Decrease in reported conversations with doctor of pharmacist when receiving prescription The percentage who had leftover pills remained high. Of those, increase in bringing leftover pills to pharmacy or other permanent disposal site. Survey findings indicate success at disseminating opioid prevention messages in the community and promoting disposal of leftover opioids. Additionally, increasing perceived risk among young adults in Alaska may predict future reductions in opioid and heroin use behaviors. Findings indicate opportunities for broader media messaging and communication with healthcare providers.
-
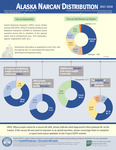
2017-2018 Infographics for the evaluation of Project HOPE
Ryan Druffel, Rebecca Porter, and Bridget Hanson
Opioid Response Programs (ORPs) across Alaska partner with DHHS, Office of Substance Misuse and Addiction Prevention (OSMAP) to distribute opioid overdose rescue kits to members of the general public and to professionals (e.g., first responders, agency/organization staff, etc.). This work consists of two infographics, and is supported by the Substance Abuse and Mental Health Services Administration (SAMHSA) grant 1H79SP022117.
-

Policy Evaluation During the Opioid Epidemic
Bridget Hanson and Jodi Barnett
This presentation provides an overview of research in Alaska's policy responses to rises in opioid use between 2016 and 2018. It outlines outcomes from qualitative analysis of interviews.
-

Promoting a Coordinated Multi-Site Evaluation for Community-Based Opioid Prevention Programs
Bridget Hanson and Jodi Barnett
The effectiveness of substance use prevention efforts is often difficult to measure over short grant cycles, especially for emerging issues such as prescription opioid misuse where data is less available and evidence-based strategies are not well understood. Coordinating state and community level evaluation efforts adds further complexity. Since 2016, six communities in Alaska, through a single federal funding stream, have worked to prevent opioid misuse among youth and young adults using policy, system, and environmental strategies. The project is focused on three key intervening variables to reduce prescription opioid misuse.The Alaska Partnerships for Success Project is funded by the Substance Abuse and Mental Health Services Administration, Center for Mental Health Services (Grant #SP020783) through the State of Alaska, Division of Behavioral Health.
-

'Please tell us about a time you administered naloxone': Maximizing data collection opportunities with challenging informants
Rebecca Porter and Bridget Hanson
This presentation provides a brief overview of results from qualitative study of Naloxone distribution and opioid overdose prevention education program in Alaska, and was presented at a meeting of the American Evaluation Association held in Minneapolis, MN, November 2019.
-

Experiences of Opioid Use Initiation and Progression among Alaskans who Use Heroin
Jodi Barnett and Bridget Hanson
The opioid epidemic has continued in Alaska and nationwide. Information about the types of opioids that are misused first, the age of first use, and the circumstances and mode of initial and progressive use of opioids can help to inform effective prevention and early intervention efforts. These topics were explored during interviews with adults in Alaska who use heroin for the Partnerships for Success project. Results indicate that most participants were exposed to opioids through a legitimate prescription in their teens to early twenties for a severe injury or multiple surgeries before developing an addiction. Some obtained prescription opioids for misuse initially from social sources such as a friend, at a party, or stealing them from a neighbor. Only two participants began their use of opioids with heroin. All participants eventually went on to use heroin which became cheaper, more effective, and easier to obtain than prescription opioids. Few participants indicated that social influences, rather than price or availability, were a factor in their transition to heroin. Recommendations and an overview of recent state prevention initiatives and policy efforts related to the findings are presented.
-

Culturally-Relevant Online Education Improves Health Workers' Capacity and Intent to Address Cancer
Katie Cueva, Mark Dignan, Laura Revels, and Melanie Cueva
-

Statute and implementation: How phantom policies affect tenure value and support
Dayna Defeo, Diane Hirshberg, and Matthew Berman
Using survey responses from public school teachers and principals in Alaska, this article describes their understanding of tenure statute, and how that understanding affected support, perceived effectiveness, and valuation of tenure. Teachers and principals who inflated tenure protections were more likely to support it; the more teachers inflated tenure protections, the higher dollar value they placed on it. The article discusses the fiscal and policy implications of tenure inflation, noting that this garners the most criticism from education reformers, but concomitantly constitutes cost savings for taxpayers.
-

Examining the sustainability potential of a multisite pilot to integrate alcohol screening and brief intervention within three primary care systems.
Diane King and Bridget Hanson
The U.S. Preventive Services Task Force recommends that clinicians adopt universal alcohol screening and brief intervention as a routine preventive service for adults, and efforts are underway to support its widespread dissemination. The likelihood that healthcare systems will sustain this change, once implemented, is under-reported in the literature. This article identifies factors that were important to post implementation sustainability of an evidence-based practice change to address alcohol misuse that was piloted within three diverse primary care organizations. The Centers for Disease Control and Prevention funded three academic teams to pilot and evaluate implementation of alcohol screening and brief intervention within multi clinic healthcare systems in their respective regions. Following the completion of the pilots, teams used the Program Sustainability Assessment Tool to retrospectively describe and compare differences across eight sustainability domains, identify strengths and potential threats to sustainability, and make recommendations for improvement. Health systems varied across all domains, with greatest differences noted for Program Evaluation, Strategic Planning, and Funding Stability. Lack of funding to sustain practice change, or data monitoring to promote fit and fidelity, was an indication of diminished Organizational Capacity in systems that discontinued the service after the pilot. Early assessment of sustainability factors may identify potential threats that could be addressed prior to, or during implementation to enhance Organizational Capacity. Although this study provides a retrospective assessment conducted by external academic teams, it identifies factors that may be relevant for translating evidence-based behavioral interventions in a way that assures that they are sustained within healthcare systems.
-

An environmental scan of the role of nurses in preventing fetal alcohol spectrum disorders.
Diane King, Bridget Hanson, Rebecca Porter, and Alexandra Edwards
Nurses are in an ideal position to talk to their patients of reproductive age about alcohol use and encourage the prevention of alcohol-exposed pregnancies. Effective conversations can be efficiently included in the clinical encounter to identify alcohol misuse and offer appropriate follow-up. This report presents results of an environmental scan of resources relevant to nursing professionals and nurses' role in addressing alcohol misuse. Gaps in nursing education and practice guidelines with regard to defining the nursing role in preventing alcohol-exposed pregnancies were revealed. Findings identified a need to promote adoption among nurses of evidence-based preventive practices to prevent alcohol misuse.
-

Implementing SBIRT in Primary Care: A Study of Three Mat-Su Borough Health Care Practices
Jessica Passini, Amanda Elkins, Diane King, and Rosyland Frazier
Despite decades of research evidence that SBIRT is effective for addressing unhealthy patterns of drinking and reducing binge drinking, its adoption within healthcare practices continues to be slow. Providers have identified numerous reasons for not routinely screening and intervening on alcohol, including limited time, training, and resources for patients requiring treatment; lack of confidence in their ability to help patients reduce their drinking; inadequate reimbursement for SBIRT services, and worry about stigmatizing patients.
-

Prevention of Fetal Alcohol Spectrum Disorders: Practice Behaviors, Attitudes, and Confidence among Members of the American College of Nurse-Midwives 2018
Rebecca Porter, Bridget Hanson, and Robyn Mertz
As part of an ACNM collaboration with the Centers for Disease Control and Prevention (CDC) and its partners and grantees on a project to prevent fetal alcohol spectrum disorders (FASDs), ACNM members were surveyed to assess the practice behaviors of certified nurse midwives and certified midwives related to the prevention of FASDs. Two surveys were conducted; the first served as a baseline from which to measure change in nurse-midwives’ and midwives’ practice behaviors over the course of the project. Results from the baseline assessment were also used to inform detailed collaborative activities between ACNM and CDC grantees whose efforts specifically target nurse-midwives (i.e., University of Alaska Anchorage (UAA); University of California, San Diego; University of Pittsburgh). The second survey was conducted 15 months after the baseline as a follow-up and findings were compared to the baseline.
-

SBIRT Utilization and Billing among Prenatal Providers in Hawaii
Stacy Tanner, Rebecca Porter, and Bridget Hanson
This report presents findings from key informant interviews that were conducted to understand Hawaii prenatal providers’ use of screening, brief intervention, and referral to treatment (SBIRT) in everyday practice. Five prenatal providers who practice in Hawaii participated in the interviews. Although participants acknowledged the importance of utilizing SBIRT in prenatal care, SBIRT appeared to be underutilized. Most did not have standard SBIRT procedures incorporated within their practice. Participants’ primary concerns regarding routine use of SBIRT included time constraints, lack of technology within the electronic health record, and stigma. Recommendations from prenatal providers regarding SBIRT decision-making, billing process improvements, and provider incentives to enhance reimbursement practices are discussed.
-

Baseline Opioid Survey: Access, Consumption, Consequences, and Perceptions among Young Adults in Alaska
Jodi Barnett, Bridget Hanson, and Oliver Smith
In September of 2015, SAMHSA awarded the Partnerships for Success (PFS) grant to the State of Alaska Department of Health and Social Services, Division of Behavioral Health (DBH). The PFS grant program is a five‐year effort that focuses on preventing and reducing substance use and building prevention capacity at both the state and community levels. DBH provides leadership for the project and facilitates the conduct of project activities by community‐level coalitions. Additionally, DBH contracted with the Center for Behavioral Health Research and Services (CBHRS) at the University of Alaska Anchorage (UAA) to conduct a comprehensive evaluation of the PFS project. Using a data‐informed prioritization process to narrow the substance abuse focus of the grant, the State Epidemiological Outcomes Workgroup chose two PFS priority areas: 1) non‐medical use of prescription opioids among 12‐25 year olds; and 2) heroin use among 18‐25 year olds. Data on the use of and consequences related to prescription opioids and heroin in Alaska are described below. Partnerships for Success (PFS) Priority Area: Non‐Medical Use of Prescription Opioids Data from the National Survey on Drug Use and Health (NSDUH) indicate that young adults aged 18‐25 consistently have the highest percentage of non‐medical use of prescription pain relievers in Alaska compared to youth aged 12‐17 and adults aged 26 and older (see Figure 1).1,2,3 While small decreases in use were observed among all age groups from 2009 to 2014, the age‐specific pattern remained consistent. Figure 1. Past year non‐medical use of prescription pain relievers in Alaska from 2009 to 2014 by age Additional data requested from NSDUH (see Table 1) indicated no significant change in non‐medical use of prescription pain reliever estimates among 12‐25 year olds in Alaska between years 2007‐2010 and 2011‐2014 but a decreasing trend was observed for past year use and past year prescription pain reliever dependence or abuse.4 0 5 10 15 2009-2010 2011-2012 2013-2014 Percentage 12-17 years 18-25 years 26+ years 4 Table 1. Past year non‐medical use of prescription pain reliever estimates among individuals aged 12 to 25 in Alaska from 2007 to 2014 1 Dependence/abuse is based on definitions found in the Diagnostic and Statistical Manual of Mental Disorders, 4th Edition (DSM‐IV) Estimates of past year non‐medical use of prescription pain relievers among individuals aged 12 and older in Alaska are slightly higher than national estimates but both follow a small decreasing trend in use from 2009 to 2014 (see Figure 2).1,2,3 Figure 2. Past year non‐medical use of prescription pain relievers among individuals aged 12 and older in the U.S. and Alaska from 2009 to 2014 Other indicators related to non‐medical use of prescription opioids in Alaska have also decreased slightly or stabilized in recent years. Treatment admissions for synthetic opiates (opiates or synthetics including Methadone, Oxycodone, or Oxycontin) as a primary, secondary, or tertiary substance of abuse have stayed relatively stable from 2013 to 2015 (1,052 to 1,011 treatment admissions), according to the Alaska Automated Information Management System (AKAIMS).5 Age‐adjusted overdose death rates in Alaska have decreased from 11.2 per 100,000 in 2009 to 8.5 per 100,000 in 2015. Although overdose deaths from prescription opioids are decreasing, Alaska still has higher rates of overdose deaths from prescription opioids than the nation overall (7.3 vs. 5.1 per 100,000 in 2012).6
-

Baseline Assessment: Alaska's Capacity and Infrastructure for Prescription Opioid Misuse Prevention
Amanda Elkins, Jodi Barnett, Bridget Hanson, and Oliver Smith
The State of Alaska Department of Health and Social Services (DHSS), Division of Behavioral Health (DBH) was awarded the Partnerships for Success (PFS) grant by the Substance Abuse and Mental Health Services Administration (SAHMSA) in 2015. DBH contracted with the Center for Behavioral Health Research and Services (CBHRS) at the University of Alaska Anchorage (UAA) to conduct a comprehensive project evaluation. As part of the evaluation, CBHRS performed a baseline assessment of the state’s capacity and infrastructure related to prescription opioid misuse prevention. Researchers conducted interviews with key stakeholders representing state government, healthcare agencies, law enforcement, substance abuse research, and service agencies. Interviews were semistructured, with questions addressing five domains of interest: (1) state climate and prevention efforts; (2) partnerships and coordinated efforts; (3) policies, practices, and laws; (4) data and data monitoring; and (5) knowledge and readiness. Thirteen interviews were conducted and analyzed using a qualitative template analysis technique combined with a SWOT analysis (i.e. strengths, weaknesses, opportunities, and threats). Emergent themes are displayed in Table 1 below. Table 1. Emergent themes from SWOT analysis Strengths Weaknesses Opportunities Threats (1) New and revised policies and guidelines (2) Activities and partnerships between state agencies and communities (3) Knowledge and awareness of state leadership (1) State policy limitations (2) Insufficient detox, treatment, and recovery support resources (3) Lack of full coordination within state agencies and with communities (1) Education enrichment (2) Policy improvements (3) Expansion of treatment, recovery, and mental health support (1) State fiscal crisis (2) Prescribing practices (3) Complexity and stigma of addiction (4) Legislative support Despite limitations in sample representativeness and interview timing, participants agreed that agencies, communities, and organizations across Alaska have demonstrated great concern about the opioid epidemic and that this concern has translated into considerable efforts to address and prevent opioid misuse. Participants also noted a variety of opportunities as targets for future work, many of which would address some of the current weaknesses that exist. Results yielded clear recommendations for increasing awareness and providing education to a variety of groups, further improving relevant policies to promote prevention, and expanding services for prevention and treatment.
-

Prevention of Fetal Alcohol Spectrum Disorders: Practice Behaviors, Attitudes, and Confidence among Members of the American College of Nurse-Midwives 2017
Bridget Hanson, Lucia Neander, and Rebecca Porter
As part of an ACNM collaboration with the Centers for Disease Control and Prevention (CDC) and its partners and grantees on a project to prevent fetal alcohol spectrum disorders (FASDs), ACNM members were surveyed to generate an assessment of practice behaviors of certified nurse-midwives and certified midwives related to the prevention of FASDs. The information will be used as a baseline from which to measure change in nurse-midwives’ and midwives’ practice behaviors over the course of the project. Results from the assessment will also be used to inform detailed collaborative activities between ACNM and CDC grantees whose efforts specifically target nurse-midwives (i.e., University of Alaska Anchorage (UAA), University of California San Diego, University of Pittsburgh).
-

Lessons Learned from Community-Based Participatory Research: Establishing a Partnership to Support Lesbian, Gay, Bisexual and Transgender Aging-in-Place.
Diane King
BACKGROUND: Due to a history of oppression and lack of culturally competent services, lesbian, gay, bisexual and transgender (LGBT) seniors experience barriers to accessing social services. Tailoring an evidence-based ageing in place intervention to address the unique needs of LGBT seniors may decrease the isolation often faced by this population. OBJECTIVE: To describe practices used in the formation of a community-based participatory research (CBPR), partnership involving social workers, health services providers, researchers and community members who engaged to establish a LGBT ageing in place model called Seniors Using Supports To Age In Neighborhoods (SUSTAIN). METHODS: A case study approach was employed to describe the partnership development process by reflecting on past meeting minutes, progress reports and interviews with SUSTAIN's partners. RESULTS: Key partnering practices utilized by SUSTAIN included (i) development of a shared commitment and vision; (ii) identifying partners with intersecting spheres of influence in multiple communities of identity (ageing services, LGBT, health research); (iii) attending to power dynamics (e.g. equitable sharing of funds); and (iv) building community capacity through reciprocal learning. Although the partnership dissolved after 4 years, it served as a successful catalyst to establish community programming to support ageing in place for LGBT seniors. CONCLUSION: Multi-sector stakeholder involvement with capacity to connect communities and use frameworks that formalize equity was key to establishing a high-trust CBPR partnership. However, lack of focus on external forces impacting each partner (e.g. individual organizational strategic planning, community funding agency perspectives) ultimately led to dissolution of the SUSTAIN partnership even though implementation of community programming was realized.
-

The Feasibility of Adopting an Evidence-Informed Tailored Exercise Program within Adult Day Services: The Enhance Mobility Program.
Diane King, S.A. Faulkner, and Bridget Hanson
This article uses the RE-AIM framework to evaluate the feasibility of implementing Enhance Mobility (EM), a tailored, evidence-informed group exercise and walking program for older adults with dementia, into an adult day services center. Participant physical performance outcomes were measured at baseline and 8 months. Program staff were interviewed to understand implementation challenges. Participant outcomes did not change significantly, though gait speed improved from limited to community ambulation levels. Implementation challenges included space reallocation and adequate staffing. Adopting EM in adult day services is feasible, and has potential to reach older adults who could benefit from tailored exercise.
-

Prevention of Fetal Alcohol Spectrum Disorders: Practice Behaviors, Attitudes, and Confidence among Members of the American College of Nurse-Midwives
Lucia Neander, Bridget Hanson, and Rebecca Porter
As part of an ACNM collaboration with the Centers for Disease Control and Prevention (CDC) and its partners and grantees on a project to prevent fetal alcohol spectrum disorders (FASDs), ACNM members were surveyed to generate an assessment of practice behaviors of certified nurse-midwives and certified midwives related to the prevention of FASDs. The information will be used as a baseline from which to measure change in nurse-midwives’ and midwives’ practice behaviors over the course of the project. Results from the assessment will also be used to inform detailed collaborative activities between ACNM and CDC grantees whose efforts specifically target nurse-midwives (i.e., University of Alaska Anchorage (UAA), University of California San Diego, University of Pittsburgh).
-

Medicaid Policies for Alcohol SBI Reimbursement
Rebecca R. Porter, Bridget Hanson, and Oliver Smith
The purpose of this report was to review existing reimbursement policies by state Medicaid agency, including the District of Columbia (D.C.), in order to understand similarities and differences associated with financial compensation for alcohol screening and brief intervention (SBI) services. Alcohol SBI is an evidence-based practice known to help reduce atrisk alcohol consumption among patients who drink too much. 1 Although alcohol SBI was designed to be a population-based approach to address unhealthy alcohol consumption, its current utilization is limited. 2 Implementation of the practice into routine clinical care remains a challenge at the health system level even with support from federal resources (e.g., SBIRT: Screening, Brief Intervention, and Referral to Treatment). One way to encourage the uptake of alcohol SBI/SBIRT among providers is to ensure that the service is reimbursable by third-party payers. However, reimbursement opportunities vary by state and payer, and in some locations are non-existent. Information about the current status of policies will assist in the development of policies and incentives to encourage healthcare providers and systems to submit claims for alcohol SBI/SBIRT and potentially increase the routine uptake of the service in clinical care
-

Medicaid Policies for Alcohol SBI Reimbursement
Oliver Smith, Bridget Hanson, and Rebecca Porter
The purpose of this report was to review existing reimbursement policies by state Medicaid agency, including the District of Columbia (D.C.), in order to understand similarities and differences associated with financial compensation for alcohol screening and brief intervention (SBI) services. Alcohol SBI is an evidence-based practice known to help reduce atrisk alcohol consumption among patients who drink too much. 1 Although alcohol SBI was designed to be a population-based approach to address unhealthy alcohol consumption, its current utilization is limited. 2 Implementation of the practice into routine clinical care remains a challenge at the health system level even with support from federal resources (e.g., SBIRT: Screening, Brief Intervention, and Referral to Treatment). One way to encourage the uptake of alcohol SBI/SBIRT among providers is to ensure that the service is reimbursable by third-party payers. However, reimbursement opportunities vary by state and payer, and in some locations are non-existent. Information about the current status of policies will assist in the development of policies and incentives to encourage healthcare providers and systems to submit claims for alcohol SBI/SBIRT and potentially increase the routine uptake of the service in clinical care.
-

Safe, Affordable, Convenient: Environmental Features of Malls and Other Public Spaces Used by Older Adults for Walking.
Diane King
BACKGROUND: Midlife and older adults use shopping malls for walking, but little research has examined mall characteristics that contribute to their walkability. METHODS: We used modified versions of the Centers for Disease Control and Prevention (CDC)-Healthy Aging Research Network (HAN) Environmental Audit and the System for Observing Play and Recreation in Communities (SOPARC) tool to systematically observe 443 walkers in 10 shopping malls. We also observed 87 walkers in 6 community-based nonmall/nongym venues where older adults routinely walked for physical activity. RESULTS: All venues had public transit stops and accessible parking. All malls and 67% of nonmalls had way finding aids, and most venues (81%) had an established circuitous walking route and clean, well-maintained public restrooms (94%). All venues had level floor surfaces, and one-half had benches along the walking route. Venues varied in hours of access, programming, tripping hazards, traffic control near entrances, and lighting. CONCLUSIONS: Despite diversity in location, size, and purpose, the mall and nonmall venues audited shared numerous environmental features known to promote walking in older adults and few barriers to walking. Future research should consider programmatic features and outreach strategies to expand the use of malls and other suitable public spaces for walking.
-

What patients want: Relevant health information technology for diabetes self-management.
Diane King
Health information technology has great potential to promote efficiency in patient care and increase patient-provider communication, and patient engagement in their treatment. This paper explored qualitatively what patients with type 2 diabetes want from electronic resources that are designed to support their diabetes self-management. Data were collected via interviews and focus groups from managed care patients who had completed participation in either a web-based (MyPath) or in-person group-based (¡Viva Bien!) longitudinal diabetes self-management study. Content analysis identified common themes that highlighted participant interest in virtual and electronic programs to support diabetes self-management goals, and their desired content and features. Eighteen ¡Viva Bien! participants completed telephone interviews and 30 MyPath participants attended seven focus groups in 2010-2011. All participants expressed a preference for face-to-face contact; however, most participants were also interested in using technology as a tool to support daily diabetes self-management decisions and to receive tailored information. Choice of technology, personalized instruction on how to use program features, and the ability to exchange information with their healthcare team were desired by all participants. Participants were divided on whether virtual social support networks should be closed to friends and family, should include other program members (peers), or should be open to anyone with diabetes. Participants aged 65 and older stressed the desire for technical support. What patients wanted from technology is real-time assistance with daily behavioral decision-making, ability to share information with their healthcare team, connections with others for support, and choice.
Printing is not supported at the primary Gallery Thumbnail page. Please first navigate to a specific Image before printing.


